- [email protected]
- +44 (0) 23 8048 3000
Calprotectin Information for Patients
Measuring faecal calprotectin levels can help doctors diagnose and monitor conditions such as inflammatory bowel disease (IBD), irritable bowel syndrome (IBS), and other gastrointestinal disorders. Patients can benefit from understanding the importance of calprotectin testing as it can potentially affect their health and quality of life. By monitoring calprotectin levels over time, healthcare providers can monitor the effectiveness of treatment and adjust treatment plans accordingly. Patients can be confident that understanding the calprotectin test can potentially help improve their health and prevent unnecessary procedures. Remember to always see your healthcare provider and follow their recommendations for testing and treatment.
In the blood, red cells perform the vital role of delivering oxygen and removing carbon dioxide from around the body by virtue of the haemoglobin they contain. The role of white cells is to help defend the body against infection and foreign substances. Calprotectin is a protein that is found in white blood cells and it has strong antibacterial and antifungal properties. There is as much calprotectin in the white cells that carry it, as there is haemoglobin in red cells.
Calprotectin is activated when inflammation occurs (whatever the cause of that may be) and thus can be used as a diagnostic indicator. The concentration of calprotectin relates directly to the severity of the inflammation. Figure 1. represents the calprotectin concentrations measured in faecal samples from patients diagnosed with Crohn’s Disease and shows increasing levels with progression of the condition.
Thus, when lower abdominal symptoms exist, a faecal calprotectin test is used to identify whether an inflammatory bowel condition that requires further investigation, is the possible cause.
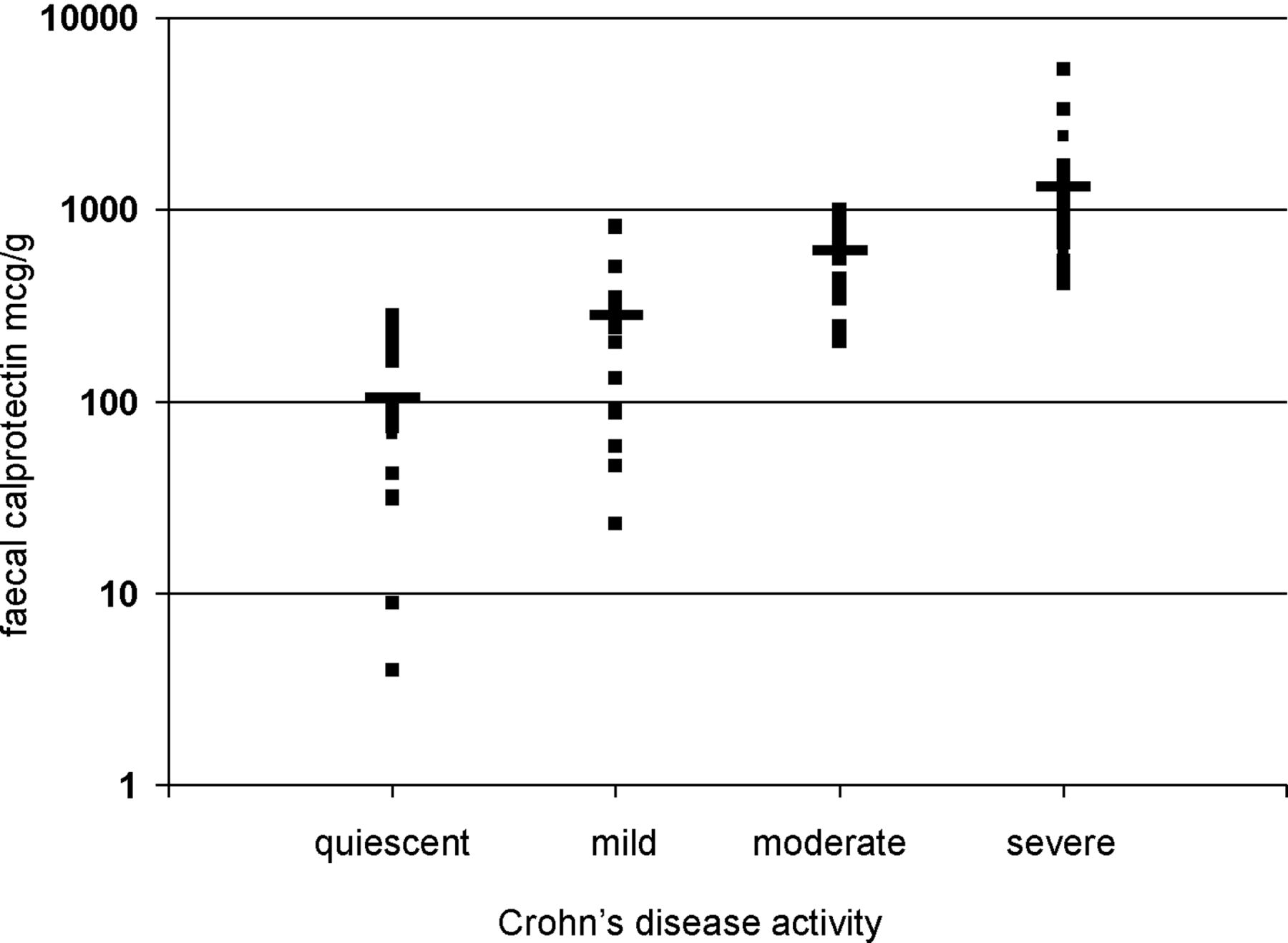
Figure 1: Faecal calprotectin levels plotted against Crohn’s disease activity (Dr James Turvill, Frontline Gastroenterology 2014)
Interpretation of Results
Faecal calprotectin testing is an extremely useful tool for the clinical team to help build up a picture of what might be causing symptoms, however it is not a specific indicator of anything other than the fact that inflammation is present somewhere in the digestive system (mouth to anus!). The challenge for the clinical team it to determine where that is coming from, and if it is significant.
In the UK, many hospitals are using the York Care Pathway, which is endorsed by BSG, NICE and Crohn’s & Colitis, for interpretation of the values obtained from a faecal calprotectin test with the following criteria:
- <100µg/g = IBD is unlikely
- 100 – 250µg/g = Intermediate result – Repeat the test in 2 weeks
- >250µg/g = Likely IBD refer to secondary care
As you can see it isn’t a clear cut yes/no result – there is an intermediate range that isn’t positive, but it is higher than a negative result should be, so other factors need to be taken into consideration.
There are a variety of things that can cause the calprotectin level to be elevated other than IBD:
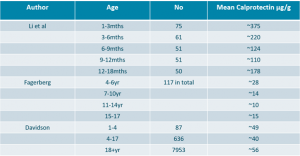
Calprotectin levels in children tend to be higher than those in adults, especially in the first few months: Davidson et al 2017 Annuals of Clinical Biochemistry
Most guidance suggests that adult cut-offs values are applicable from 4 years onwards.
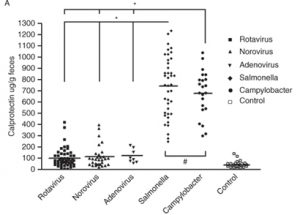
Bacterial infections can cause transient rises in calprotectin levels; viral infections, don’t tend to cause significant increases: Chen et al 2012
Other publications have reported significantly lower calprotectin levels even for bacterial infections, so the calprotectin level is probably also related to the specific causative agent (some bacteria are more pathogenic than others), the severity of the disease and the age of the patient (the study above was paediatric who can have higher levels anyway).
Things that cause an irritation of the gastric system and hence an inflammatory response will cause the calprotectin levels to rise:
-
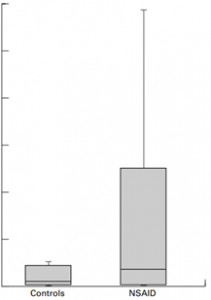
- Some medication, especially if they are in prolonged use e.g. NSAIDs – aspirin and ibuprofen: Tibble et al 1999 Gut. (See image)
- Excessive alcohol
- Ulcers
- Carcinoma
Proton pump inhibitors have been associated with higher calprotectin levels: Poullis et al 2003 Correspondence European J Gastro & Hept.
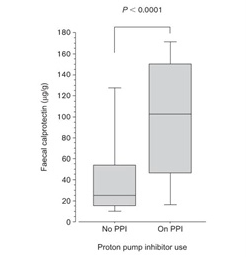
In the literature there are also a number of other conditions that may (or may not) cause the calprotectin levels to rise e.g. untreated allergies or coeliac disease, pancreatitis, appendicitis, mild diverticulitis, ankylosing spondylitis. Studies differ in their conclusions, but the levels are also not usually as high as that seen with IBD.

How to Take a Sample for Faecal Calprotectin Testing:
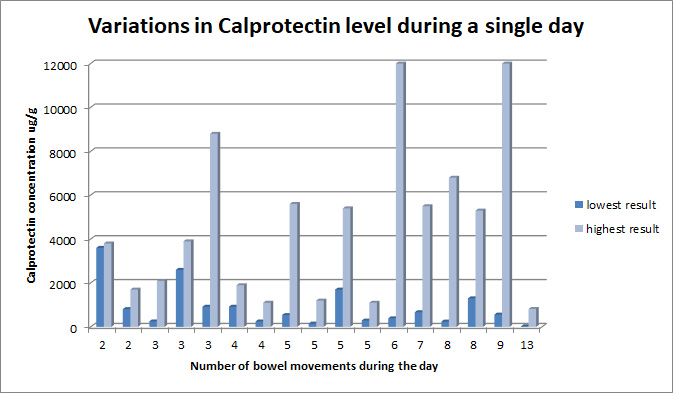
Calprotectin enters the stool whilst it is contact with the gut wall, and the concentration will vary depending on the transit time of the gut contents. If things are moving rapidly then it may not collect much calprotectin! For this reason it is recommended that the first stool of the day is used – this is likely to have been in the gut overnight and so should contain the highest level of calprotectin. If the first stool isn’t possible then use a sample where there has been a reasonable time between bowel movements.
Empty the bladder before collecting the sample to avoid contamination and dilution with urine. The sample must not come into contact with the toilet water which may contain chemicals that could influence the test result.
Methods for Collecting a Stool Sample:
- Fe-Col – a paper loop that fits around the toilet seat and can be flushed away when finished.
Watch the video - Put cling film (loosely to form a dip but not touching the water) under the toilet seat, attached to the porcelain and put the seat back down. Once the sample has been taken the excess can be allowed to fall into the toilet for disposal. Do NOT flush the cling film as this will cause blockages
- Use a clean take away container, foil dish or paper plate to catch the sample. Excess sample can be tipped into the toilet, and the container disposed of appropriately
- Lift the seat and place a cat litter bag (or other large opening plastic bag) over the porcelain and put the seat back down to hold in place whilst the sample is taken. Excess sample can be tipped into the toilet but the bag must not be flushed

Calprotectin is not evenly distributed in the stool sample, so a sensible amount needs to be sent to the laboratory for testing – too little and there may be no calprotectin in the portion sent. Half fill the sample container with stool and seal tightly – ensure your full name and the date is on the pot. Please don’t completely fill the container in case of leaks!
Return the sample to the surgery/hospital within 24 hours.
PLEASE NOTE: The information on this site is primarily designed for use by healthcare professionals rather than the general public. Similarly the products are not suitable for personal purchase and self-testing without direction from a doctor. If you have any concerns about Calprotectin testing or IBD, IBS and related conditions, please speak to your GP.